CARDIAC TAMPONADE
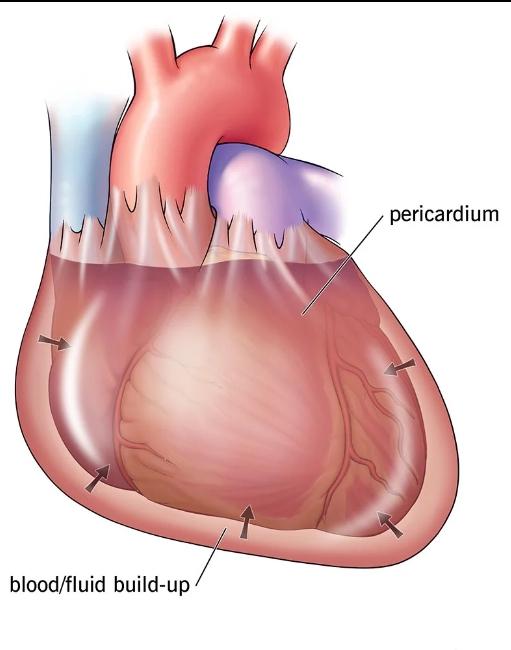
Cardiac tamponade is a medical emergency that takes place when abnormal amounts of fluid accumulate in the pericardial sac, compressing the heart and leading to a decrease in cardiac output and shock.
Cardiac tamponade is caused by the build up of pericardial fluid (blood, exudate fluid, or transudate fluid) that can accumulate for several reasons. Hemorrhage, such as from a penetrating wound to the heart or ventricular wall rupture after an MI, can lead to a rapid increase in pericardial volume. Other risk factors, which tend to produce a slower-growing effusion, include infection (tuberculosis [TB], myocarditis), autoimmune diseases, neoplasms, uremia, and other inflammatory diseases (pericarditis).
The diagnosis of Cardiac tamponade can be achieved via Physical examination, Electrocardiography, Heart catheterization, Echocardiography, Chest X-ray, and Chest CT..
A hallmark sign of cardiac tamponade is a trio of symptoms known as Beck’s triad:
First described in 1935 by the American cardiothoracic surgeon, Claude Beck.
1. Low blood pressure (Hypotension).
2. Distension of the jugular veins.
3. Muffled or diminished heart sounds on cardiac auscultation.
TREATMENT: Echocardiographically-guided pericardiocentesis with catheter drainage, an invasive procedure used to avoid unnecessary surgery.





Responses